Tongue diagnosis in Chinese medicine
On this page
- What is tongue diagnosis?
- The tongue map — organ zones
- Tongue body colour
- Tongue body shape and size
- Tongue coating
- Tongue moisture
- Tongue movement
- Sublingual veins
- Common tongue patterns and what they mean
- Tongue diagnosis in my practice
- Commonly asked questions about tongue diagnosis
1. What is tongue diagnosis?
Tongue diagnosis is one of the most important and distinctive diagnostic tools in traditional Chinese medicine (TCM). Along with pulse diagnosis, it forms the cornerstone of the TCM physical examination and provides a direct window into the state of the body's internal organ systems, qi, blood and fluids.
The tongue is considered an exceptionally reliable diagnostic indicator in TCM because it is a highly vascular structure whose colour, shape, coating and moisture are continuously influenced by changes in the internal organs. Unlike symptoms — which can be subjective and variable — the tongue provides objective, visible evidence of what is happening inside the body. A skilled TCM practitioner can detect patterns of disharmony from tongue examination that may not yet be producing significant symptoms, making tongue diagnosis a valuable tool for early identification of imbalance.
The practice of tongue diagnosis in Chinese medicine dates back over two thousand years. It was systematically codified in the classical texts of the Song and Ming dynasties and refined further in the Qing dynasty, when dedicated tongue diagnosis atlases were compiled documenting hundreds of distinct tongue presentations and their corresponding internal patterns. This rich clinical tradition, refined across centuries of continuous observation, underpins the tongue diagnosis practice used in TCM clinics today.
In contrast to western medicine, where the tongue is examined primarily for signs of infection or vitamin deficiency, TCM tongue examination is a sophisticated multi-parameter assessment. A TCM practitioner examines the tongue body colour, the tongue body shape and size, the nature and distribution of the tongue coating, the moisture level, the presence of any markings or features, and any movement or trembling — each of which yields distinct diagnostic information.
2. The tongue map — organ zones
One of the foundational principles of TCM tongue diagnosis is that different areas of the tongue correspond to different internal organ systems. This mapping allows the practitioner to localise patterns of disharmony to specific organs by observing where on the tongue particular features — such as changes in colour, coating thickness or surface markings — are concentrated.
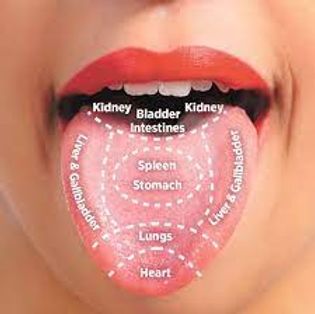
The conventional TCM tongue map divides the tongue into five primary zones:
- Tip of the tongue — reflects the state of the Heart and, to a lesser extent, the Lungs. Redness at the tip is one of the most commonly observed findings in clinical practice and typically indicates Heart fire or Liver fire rising, often associated with anxiety, insomnia or emotional disturbance.
- Front third (behind the tip) — corresponds to the Lungs. Pale or white discolouration in this zone, or the presence of a thick white coating, can indicate Lung qi deficiency or the presence of cold or phlegm in the Lungs.
- Centre of the tongue — reflects the state of the Spleen and Stomach, the central organs of digestion and transformation in TCM. A thick, greasy coating concentrated in the centre is a common indicator of Spleen dampness or Stomach phlegm. Cracks in the centre of the tongue often indicate Stomach yin deficiency.
- Sides of the tongue — correspond to the Liver and Gallbladder. Redness, swelling or purple discolouration on the sides of the tongue may indicate Liver qi stagnation, Liver fire or Liver blood stasis — conditions that are frequently associated with chronic stress, emotional suppression and hormonal imbalance.
- Root of the tongue — reflects the state of the Kidneys and Bladder, and to some extent the lower Jiao (lower body). A particularly thick or absent coating at the root can indicate Kidney yin deficiency or accumulation of dampness in the lower body.
These zone correspondences are not rigid boundaries but overlapping regions of clinical emphasis. The tongue is examined as a whole, and the pattern that emerges from considering all zones together — alongside all other tongue features — is what informs the TCM diagnosis.
3. Tongue body colour
The colour of the tongue body — the muscular tissue of the tongue itself, as distinct from its coating — is one of the most important parameters in tongue diagnosis. It reflects the state of qi, blood and yin in the body.
- Pale pink — the normal, healthy tongue colour. Indicates a balanced state of qi and blood with no significant internal disharmony.
- Pale or white tongue body — indicates deficiency of qi, yang or blood. A pale tongue is commonly seen in patients with fatigue, coldness, poor circulation, anaemia or constitutional weakness. Yang deficiency — often accompanied by cold extremities and low energy — typically produces a very pale, moist tongue.
- Red tongue body — indicates heat in the body. This may be full heat (excess fire from an external pathogen or emotional excess) or empty heat (deficiency heat arising from yin deficiency, where the cooling, moistening yin is insufficient to control the body's yang). A red tongue with a yellow coating suggests full heat; a red tongue without coating, or with a very thin coating, suggests yin deficiency heat.
- Crimson or deep red tongue body — indicates a more severe degree of heat, particularly heat that has penetrated deeply into the blood level or ying level. This is seen in febrile illness, severe yin deficiency or blood-level heat.
- Purple tongue body — indicates blood stasis — poor circulation and blood that is not moving freely through the vessels. A purple tongue may be bluish-purple (cold stagnation) or reddish-purple (heat stagnation). Blood stasis of the tongue is frequently associated with chronic pain, cardiovascular conditions, gynaecological problems including painful periods, endometriosis and fibroid formation, and prolonged emotional suppression.
- Blue tongue body — a relatively rare finding indicating severe cold constriction of the vessels or profound blood stasis with cold.
4. Tongue body shape and size
The shape and size of the tongue body provide additional diagnostic information about the underlying state of the body's fluids, qi and organ systems.
- Normal size and shape — a tongue of moderate size, neither swollen nor shrunken, that fits comfortably within the mouth without being pressed against the teeth.
- Swollen or enlarged tongue — indicates the presence of dampness, phlegm or fluid accumulation in the body. Dampness in TCM arises from impaired Spleen function and manifests as sluggishness, heaviness, digestive bloating, excess mucus and fatigue. A swollen tongue that leaves tooth marks on its sides (a scalloped edge) is one of the most common clinical findings and is a reliable indicator of Spleen qi deficiency with dampness.
- Thin or shrunken tongue — indicates deficiency of yin, blood or body fluids. A thin, dry tongue that appears shrunken or contracted suggests significant yin or blood deficiency.
- Stiff or rigid tongue — may indicate wind invasion, liver wind or phlegm obstructing the heart orifices, and may be associated with difficulty speaking clearly.
- Flaccid or soft tongue — a tongue that appears soft and lacking tone indicates severe qi, blood or yin deficiency.
- Cracked tongue — cracks in the tongue surface indicate deficiency of fluids or yin. Long central cracks are associated with Heart or Stomach issues; cracks across the tongue may indicate chronic Stomach yin deficiency. It is worth noting that some cracks are constitutional and present throughout life without pathological significance; the key is to assess changes over time.
- Scalloped edges (tooth marks) — indentations along the sides of the tongue created by the teeth are a very common finding and reliably indicate Spleen qi deficiency with dampness. This pattern is associated with fatigue, digestive weakness, bloating and a tendency to retain fluid.
5. Tongue coating
The tongue coating — also called the tongue fur or moss — is the layer that covers the tongue surface and is produced by the Stomach. The nature, thickness, colour and distribution of the tongue coating provide important information about the state of the digestive system, the presence of external pathogens, and the degree and nature of any internal heat, cold, dampness or dryness.
- Normal coating — a thin, white, evenly distributed coating that is slightly moist. This indicates a healthy Stomach and the absence of significant pathogenic factors.
- Thin white coating — normal or may indicate the early stage of an external cold invasion.
- Thick white coating — indicates the presence of cold, dampness or phlegm in the interior. Commonly seen in patients with digestive sluggishness, excess mucus, sinus congestion or respiratory phlegm.
- Thick yellow coating — indicates interior heat. A yellow coating results from heat transforming the coating from white to yellow. A thick, greasy yellow coating indicates damp-heat, a common pattern in inflammatory digestive conditions, skin disorders and gynaecological infections.
- Grey or black coating — indicates extreme interior cold (grey-black moist coating) or extreme interior heat (grey-black dry coating). These are relatively uncommon findings in modern clinical practice.
- Greasy or sticky coating — indicates the presence of phlegm or dampness regardless of colour. A greasy coating is one of the key diagnostic indicators of a damp or phlegm pattern.
- Dry coating — indicates deficiency of body fluids or yin, or the presence of heat consuming fluids.
- Peeled coating (geographic tongue) — areas where the coating is absent or has peeled away indicate deficiency of Stomach yin. A completely coating-free, shiny tongue (mirror tongue) indicates severe yin deficiency.
- Rootless coating — a coating that can be scraped off easily and appears to be sitting on the surface of the tongue rather than growing from it indicates that stomach qi is becoming deficient.
6. Tongue moisture
The degree of moisture on the tongue reflects the state of the body's fluids and the balance between yin (cooling, moistening) and yang (warming, drying) forces.
- Normal moisture — the tongue is slightly moist but not excessively wet.
- Wet or dripping tongue — indicates yang deficiency or cold, where the yang is insufficient to metabolise and transform fluids. Excess fluid accumulates and manifests as a wet tongue.
- Dry tongue — indicates yin deficiency, heat consuming fluids, or insufficient production of body fluids. A dry tongue is often seen in patients with chronic illness, post-menopausal heat symptoms or prolonged use of diuretics.
7. Tongue movement
Observation of how the tongue moves when it is extended can provide additional diagnostic information, particularly in relation to internal wind and the nervous system.
- Normal movement — the tongue extends smoothly in the midline without deviation or trembling.
- Trembling or quivering tongue — indicates Liver wind, qi or blood deficiency, or, if accompanied by red colour, Liver fire generating wind.
- Deviation to one side — indicates internal wind or phlegm obstructing the channels and may be associated with neurological conditions.
- Tongue rolling inward — indicates extreme heat consuming fluids or Liver wind in acute febrile conditions.
8. Sublingual veins
Examination of the underside of the tongue — specifically the two sublingual veins that run beneath the tongue on either side of the frenulum — provides important information about blood circulation. Normally these veins are barely visible or a light blue-green colour. Prominent, dark purple, distended or tortuous sublingual veins are a reliable indicator of blood stasis, particularly in the chest or lower abdomen. This finding is clinically significant in patients with cardiovascular conditions, chronic pain, gynaecological disorders and conditions involving poor peripheral circulation.
9. Common tongue patterns and what they mean
In clinical practice, tongue features are never assessed in isolation — they are interpreted as part of a combined picture alongside the patient's symptoms and the findings of pulse diagnosis. The following are some of the most commonly encountered tongue patterns in TCM practice.
- Pale, slightly swollen, with scalloped edges and thin white coating — indicates Spleen qi deficiency with dampness. This is the single most commonly seen tongue pattern in clinical practice in the UK. It is associated with fatigue, digestive weakness, loose stools or bloating, cold extremities, and a tendency to gain weight or retain fluid.
- Red tip with normal body — indicates Heart fire or Liver fire rising. This very common finding is associated with anxiety, palpitations, insomnia and emotional agitation.
- Red body, thin or no coating — indicates yin deficiency with empty heat. Common in menopausal patients, those with chronic fatigue, or anyone who has depleted their yin through overwork, insufficient sleep or chronic stress.
- Red body with thick yellow greasy coating — indicates damp-heat. Associated with inflammatory digestive conditions, skin disorders such as acne, pelvic infections, and conditions such as IBS with inflammatory features.
- Purple body with or without dark coating — indicates blood stasis. Associated with chronic pain, cardiovascular disease, gynaecological conditions including painful periods, endometriosis and fibroids, and longstanding emotional suppression.
- Pale body, dry, thin — indicates blood deficiency. Common in women with heavy or prolonged periods, post-partum patients, or those with nutritional deficiency.
- Central crack reaching the tip — indicates Heart yin deficiency or a constitutional weakness of the Heart, often associated with anxiety, restless sleep and emotional sensitivity.
10. Tongue diagnosis in my practice
Tongue examination is an integral part of every consultation in my practice. At your initial appointment I will ask you to extend your tongue while I observe all of the features described above. You do not need to hold your tongue out for long — a few seconds is sufficient for an experienced practitioner to register the key findings.
I encourage patients to observe their own tongues regularly between appointments. Changes in the tongue can reflect how the body is responding to treatment, seasonal changes, dietary changes, emotional stress and fluctuations in health. Many patients find it illuminating to photograph their tongue periodically and compare changes over time.
It is worth noting that certain foods, drinks and medications can temporarily affect tongue colour and coating. Coffee, tea and coloured foods or drinks can stain the tongue coating; antibiotics and some other medications can affect the coating significantly. I always ask patients about recent food and drink intake before interpreting tongue findings, and a single examination should always be considered in the context of the patient's complete clinical picture.
Tongue diagnosis works in conjunction with pulse diagnosis, detailed case-taking and the full range of TCM observational techniques to build an accurate picture of the patient's pattern of disharmony. It is this individualised pattern that forms the basis of the tailored treatment plan.
11. Commonly asked questions about tongue diagnosis
Can I self-diagnose from my own tongue?
You can learn to observe basic tongue features — such as scalloped edges, a very red tip or a thick coating — and these observations can give you useful general information about your health. However, accurate TCM tongue diagnosis requires training and experience, and must always be interpreted in the context of the full clinical picture including symptoms, history and pulse findings. Self-observation is a useful adjunct to, not a substitute for, professional assessment.
Does my tongue change from day to day?
Yes — the tongue changes continuously in response to your health, diet, emotional state, sleep quality and treatment. This is precisely what makes it such a valuable diagnostic tool: it provides a real-time window into the body's current state. Changes in the tongue over the course of a treatment programme are one of the ways I assess whether treatment is having its intended effect.
Why does my practitioner need to see my tongue at every appointment?
Because the tongue reflects the current state of your internal organs and body fluids, it changes as your health changes. Tracking how your tongue evolves over the course of treatment — for example, whether a thick coating is clearing, whether redness is reducing, or whether a very pale tongue is returning to a healthier colour — is one of the most reliable ways to assess progress and refine the treatment plan accordingly.
Does wearing lipstick or eating affect my tongue examination?
Yes. I always ask patients to remove lipstick before examination and to avoid eating strongly coloured foods immediately before their appointment where possible. Coffee, tea, coloured sweets and some medications can all temporarily stain the coating and affect the colour of the tongue body. If there is any uncertainty about whether a finding is genuine or due to external staining, I will take this into account in my assessment.
Is tongue diagnosis the same in all traditions of Chinese medicine?
The core principles of tongue diagnosis are shared across the major traditions of East Asian medicine — including Chinese, Japanese and Korean styles. Some schools place greater emphasis on tongue diagnosis relative to pulse diagnosis, and there are some differences in the interpretation of specific findings between schools. The system described on this page reflects mainstream TCM tongue diagnosis as taught and practised in China and in UK TCM institutions.
References
- Maciocia, G. (1995). Tongue Diagnosis in Chinese Medicine (revised ed.). Seattle: Eastland Press.
- Maciocia, G. (2015). The Foundations of Chinese Medicine (3rd ed.). Edinburgh: Churchill Livingstone.
- Huang Di Nei Jing Su Wen (The Yellow Emperor's Classic of Internal Medicine). (~300 BCE). Beijing: People's Medical Publishing House.
- Wang, S. (1341). Ao Shi Shang Han Jin Jing Lu (The Golden Mirror of Cold Damage). Translated and discussed in Maciocia (1995).
- Porkert, M. (1974). The Theoretical Foundations of Chinese Medicine. Cambridge, MA: MIT Press.
- Scheid, V., Bensky, D., Ellis, A., & Barolet, R. (2009). Chinese Herbal Medicine: Formulas and Strategies (2nd ed.). Seattle: Eastland Press.




















